Varicose veins are a common condition, and they necessitate medical intervention for proper management. Medical professionals provide specific coping strategies based on clinical evidence. Understanding the underlying mechanisms helps patients make informed decisions about their health. Here is more information on this condition, what causes it, the symptoms, how to cope, and the benefits of professional guidance:
What Are Varicose Veins?
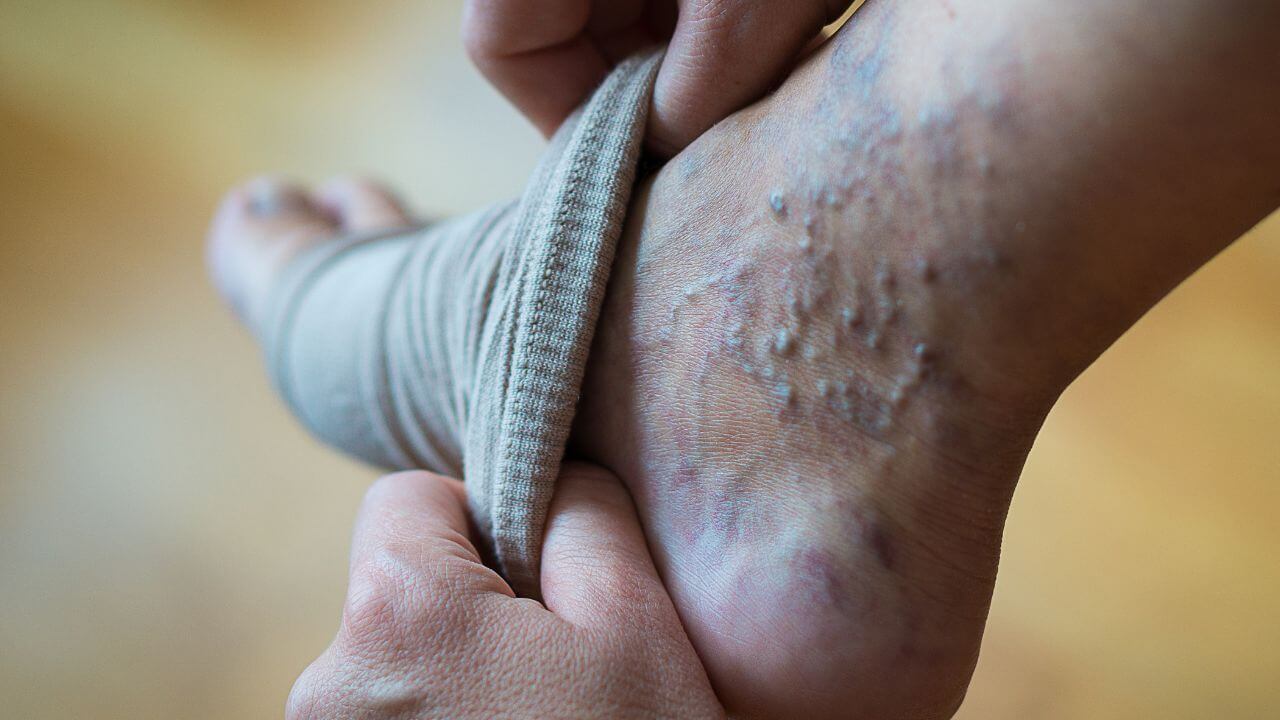
Varicose veins are enlarged blood vessels that typically appear twisted or bulging under the skin. They most commonly develop in the legs due to the increased pressure of standing or walking. The veins become visible on the skin’s surface, and patients may notice them during routine physical observation.
These abnormal veins indicate an issue with blood circulation, and the condition is known clinically as chronic venous insufficiency. The structural integrity of the blood vessel changes over time. The vessel walls stretch beyond their normal capacity, resulting in the characteristic swelling associated with the condition.
What Causes Them?
Blood travels through the veins to the heart, and small valves prevent the blood from flowing backward. When these valves become weak, blood pools in the affected veins. The pooling increases internal pressure within the vessel. The vein expands and twists over time due to this continuous strain.
Several factors contribute to this valve malfunction, with age being a primary contributor. Veins lose elasticity over time, and the structural integrity of the valves diminishes with natural aging. Additional factors include genetics and prolonged standing or sitting.
What Are the Symptoms?
Patients may report visible dark purple or blue veins that appear like cords on the legs. Physical discomfort sometimes accompanies the visual signs of the condition. Aching or heavy feelings in the legs are common, and pain may worsen after prolonged sitting or standing.
Some individuals experience muscle cramping or swelling in the lower legs, and this has the potential to lead to additional mobility issues. Itching around one or more of the veins occurs in some cases. Skin discoloration can develop around a varicose vein in advanced cases. These symptoms vary in severity, prompting individuals to seek medical evaluation.
How Can You Cope?
Patients manage symptoms through conservative lifestyle modifications that help improve overall blood flow. Elevating the legs above heart level reduces venous pressure. Regular physical activity improves circulation in the lower extremities, and walking is recommended for symptom management. Compression stockings apply steady pressure to the legs, and this helps veins and leg muscles move blood more efficiently.
How Is Professional Guidance Beneficial?
A cardiologist thoroughly evaluates the cardiovascular system and assesses the severity of venous insufficiency. This specialized assessment determines the most appropriate treatment plan for the patient. Diagnostic tools like ultrasound provide clear images of blood flow, and the cardiologist can identify specific damaged valves using these techniques. Medical intervention becomes necessary for advanced cases, and cardiologists may perform various minimally invasive procedures.
Seek Professional Advice Today
Coping with this condition requires understanding the symptoms, and a medical evaluation can provide effective management options. Conservative management may offer relief for mild symptoms. Specialized medical treatments help resolve more severe cases. Contact a specialized clinic to schedule a comprehensive evaluation and discuss your specific treatment options with a cardiologist.